- English
- Esta página
- Página inicial
- Arabic (اللغة العربية)
- Chinese (简体中文)
- French (Français)
- Haitian Creole (Kreyòl Ayisyen)
- Hindi (जानकारी)
- Korean (한국어)
- Polish (język polski)
- Portuguese (Português)
- Russian (Русский)
- Spanish (Español)
- Tagalog (Tagalog)
- Ukrainian (Українська)
- Vietnamese (Tiếng Việt)
- All Languages
Español
PDFs by language
Our 24/7 cancer helpline provides information and answers for people dealing with cancer. We can connect you with trained cancer information specialists who will answer questions about a cancer diagnosis and provide guidance and a compassionate ear.
![]()
Chat live online
Select the Live Chat button at the bottom of the page
Our highly trained specialists are available 24/7 via phone and on weekdays can assist through video calls and online chat. We connect patients, caregivers, and family members with essential services and resources at every step of their cancer journey. Ask us how you can get involved and support the fight against cancer. Some of the topics we can assist with include:
- Referrals to patient-related programs or resources
- Donations, website, or event-related assistance
- Tobacco-related topics
- Volunteer opportunities
- Cancer Information
For medical questions, we encourage you to review our information with your doctor.
Surgery for Cervical Cancer
Many women with cervical cancer will have some type of surgery. Surgery can be used to:
- Help diagnose cervical cancer
- Help determine how far the cancer has spread
- Help treat the cancer (especially for early-stage cancers)
Surgery for cervical pre-cancers
Two types of procedures can be used to treat pre-cancers of the cervix:
- Ablation destroys cervical tissue with cold temperatures or with a laser rather than removing it.
- Excisional surgery (conization) cuts out and removes the pre-cancer.
Cryosurgery
Cryosurgery is a type of ablation where a very cold metal probe is placed directly on the cervix. This kills the abnormal cells by freezing them. It is used to treat cervical intraepithelial neoplasia (CIN). This can be done in a doctor’s office or clinic. After cryosurgery, you may have a watery brown discharge for a few weeks.
Laser ablation
Laser ablation directs a focused laser beam through the vagina to vaporize (burn off) abnormal cells. This might be done in a doctor’s office under local anesthesia (numbing medicine) or in the operating room with general anesthesia since it can cause more discomfort than cryotherapy. It is also used to treat cervical intraepithelial neoplasia (CIN).
Conization
Another way to treat cervical intraepithelial neoplasia (CIN) is with excisional surgery called conization. The doctor removes a cone-shaped piece of tissue from the cervix. The tissue removed in the cone includes the transformation zone where cervical pre-cancers and cancers are most likely to start. A cone biopsy is not only used to diagnose pre-cancers and cancers. It can also be used as a treatment since it can sometimes completely remove pre-cancers and some very early cancers.
The procedure can be done in different ways:
- Using a surgical blade (cold knife cone biopsy)
- Using a laser beam (laser conization)
- Using a thin wire heated by electricity (the loop electrosurgical excision procedure, LEEP or LEETZ procedure).
Surgery for invasive cervical cancer
Procedures to treat invasive cervical cancer are:
- Hysterectomy (simple or radical)
- Trachelectomy
Simple hysterectomy
A simple hysterectomy removes the uterus (both the body of the uterus and the cervix) but not the structures next to the uterus (parametria and uterosacral ligaments). The vagina and pelvic lymph nodes are not removed. The ovaries are usually left in place unless there is another reason to remove them.
Simple hysterectomy can be used to treat certain types of severe CIN or certain types of very early cervical cancer.
There are different ways to do a hysterectomy:
- Abdominal hysterectomy: The uterus is removed through a surgical incision in the front of the abdomen.
- Vaginal hysterectomy: The uterus is removed through the vagina.
- Laparoscopic hysterectomy: The uterus is removed using laparoscopy. First, a thin tube with a tiny video camera at the end (the laparoscope) is inserted into one or more very small surgical incisions made on the abdominal wall to see inside the abdomen and pelvis. Small instruments can be controlled through the tube(s), so the surgeon can cut around the uterus without making a large cut in the abdomen. The uterus is then removed through a cut in the vagina.
- Robotic-assisted surgery: In this approach, the laparoscopy is done with special tools attached to robotic arms that are controlled by the doctor to help perform precise surgery.
General anesthesia is used for all of these operations.
For a laparoscopic or vaginal hysterectomy, the hospital stay is usually 1 to 2 days, followed by a 2- to 3-week recovery period. A hospital stay of 3 to 5 days is common for an abdominal hysterectomy, and complete recovery takes about 4 to 6 weeks.
Possible side effects: Any type of hysterectomy results in infertility (inability to have children). Complications are unusual but could include bleeding, infection, or damage to the urinary or intestinal systems such as the bladder or colon.
Hysterectomy does not change a woman's ability to feel sexual pleasure. A woman does not need a uterus or cervix to reach orgasm. The area around the clitoris and the lining of the vagina remain as sensitive as before a hysterectomy. More information about managing the sexual side effects of cervical cancer treatment can be found in Sex and the Woman with Cancer.
Radical hysterectomy
For this operation, the surgeon removes the uterus along with the tissues next to the uterus (the parametria and the uterosacral ligaments), the cervix, and the upper part (about 1 inch [2-3cm]) of the vagina next to the cervix. The ovaries are not removed unless there is some other medical reason to do so. More tissue is removed in a radical hysterectomy than in a simple one, so the hospital stay can be longer. Some lymph nodes will also be removed and checked for cancer at this time.
This surgery is usually done through a large abdominal incision (also known as open surgery). Often, some pelvic lymph nodes are removed as well. (This procedure, known as lymph node dissection, is discussed later in this section.)
A radical hysterectomy can also be done using laparoscopy or robot-assistance. (See the Simple hysterectomy section for a description of laparoscopy.) These techniques are also referred to as minimally invasive surgery. Laparoscopic (or robotic) surgery can result in less pain, less blood loss during the operation, and a shorter hospital stay compared to open surgery. However, it is very important to note that recent studies have shown that women who have minimally invasive radical hysterectomies for cervical cancer have a higher chance of the cancer recurring and a higher risk of dying from the cancer than those who have surgery through an abdominal incision (open surgery). Having a radical hysterectomy through an abdominal cut is the preferred type of surgery in most cases. Laparoscopic surgery may still be an option for a small specific group of women with early stage cancer, but you should discuss your options carefully with your doctor.
A modified radical hysterectomy is similar to a radical hysterectomy but does not remove as much of the vagina and tissues next to the uterus (the parametria and the uterosacral ligaments) and lymph nodes are usually not removed.
Possible side effects: Because the uterus is removed, this surgery results in infertility. Because some of the nerves to the bladder are removed, some women have problems emptying their bladder after this operation and may need a catheter for a time. Complications are unusual but could include bleeding, infection, or damage to the urinary and intestinal systems such as the bladder or colon.
Removal of some of the lymph nodes to check for cancer may sometimes result in lymphedema (leg swelling). This is not common, but may happen after surgery and treated with different methods.
Radical hysterectomy does not change a woman's ability to feel sexual pleasure. Although the vagina is shortened, the area around the clitoris and the lining of the vagina is as sensitive as before. A woman does not need a uterus or cervix to reach orgasm. When cancer has caused pain or bleeding with intercourse, the hysterectomy may actually improve a woman's sex life by stopping these symptoms. More information about managing the sexual side effects of cervical cancer treatment can be found in Sex and the Woman with Cancer.
Trachelectomy
A radical trachelectomy, allows women to be treated without losing their ability to have children. The operation is done either through the vagina or the abdomen, and is sometimes done using laparoscopy.
This procedure removes the cervix and the upper part of the vagina but not the body of the uterus. The surgeon then places a permanent "purse-string" stitch inside the uterine cavity to keep the opening of the uterus closed, the way the cervix normally would.
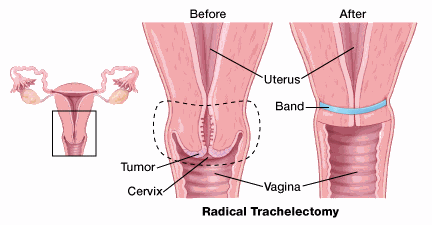
The nearby lymph nodes are also removed using laparoscopy which may require another incision (cut). The operation is done either through the vagina or the abdomen.
After trachelectomy, some women are able to carry a pregnancy to term and deliver a healthy baby by cesarean section, although women who have had this surgery might have a higher risk of miscarriage.
Pelvic exenteration
This operation is done for very specific cases of recurrent cervical cancer. In this surgery, all of the same organs and tissues are removed as in a radical hysterectomy with pelvic lymph node dissection. (Lymph node dissection is discussed in the next section.) In addition, the bladder, vagina, rectum, and part of the colon is also removed, depending on where the cancer has spread.
If your bladder is removed, you will need a new way to store and get rid of urine. This usually means using a short piece of intestine to function as a new bladder. The new bladder may be connected to the abdominal wall so that urine is drained periodically when the patient places a catheter into a urostomy (a small opening). Or urine drains continuously into a small plastic bag attached to the front of the abdomen. For more information, see Urostomy Guide.
If the rectum and part of the colon are removed, a new way to get rid of solid waste must be created. This is done by attaching the remaining intestine to the abdominal wall so that fecal material can pass through a small opening (stoma) into a small plastic bag worn on the front of the abdomen (more information about colostomies can be found in Colostomy Guide). In some cases, it may be possible to remove the cancerous part of the colon (next to the cervix) and reconnect the colon ends so that no bags or external appliances are needed.
If the vagina is removed, a new vagina can be surgically made out of skin, intestinal tissue, or muscle and skin (myocutaneous) grafts.
Sexual impact of pelvic exenteration
Recovery from total pelvic exenteration takes a long time. Most women don't begin to feel like themselves again for about 6 months after surgery. Some say it takes a year or two to adjust completely.
Nevertheless, these women can lead happy and productive lives. With practice, they can also have sexual desire, pleasure, and orgasms.
More information about managing the sexual side effects of cervical cancer treatment can be found in Sex and the Woman with Cancer.
Surgery to remove nearby lymph nodes
Para-aortic lymph node sampling
Usually during surgery for a radical hysterectomy, the lymph nodes next to the aorta (the large artery in the abdomen) are removed. This is called para-aortic lymph node sampling. The lymph nodes may be sent to the lab during the operation for quick testing. If the para-aortic lymph nodes show cancer, the surgery may be stopped, and radiation and chemotherapy given instead. If the lymph nodes do not show cancer, then pelvic lymph nodes (see below) are usually removed and the radical hysterectomy completed. Any tissue removed during surgery will be tested to see if the cancer has spread there. If so, radiation therapy with or without chemotherapy might be recommended.
Pelvic lymph node dissection
Cancer that starts in the cervix can spread to lymph nodes (pea-sized collections of immune system cells) in the pelvis. To check for lymph node spread, the surgeon might remove some of these lymph nodes. This procedure is known as a pelvic lymph node dissection or lymph node sampling. It is done at the same time as a hysterectomy or trachelectomy.
Removing lymph nodes can lead to fluid drainage problems in the legs. This can cause severe leg swelling, a condition called Lymphedema.
Sentinel lymph node mapping and biopsy
Sentinel lymph node mapping and biopsy is a procedure in which the surgeon finds and removes only the lymph node(s) where the cancer would likely spread first. To do this, the surgeon injects a radioactive substance and/or a blue dye into the cervix at the beginning of the surgery. Lymphatic vessels will carry these substances along the same path that the cancer would likely take. The first lymph node(s) the dye or radioactive substance travels to will be the sentinel node(s). Removing only one or a few lymph nodes lowers the risk of side effects from the surgery, such as leg swelling that is also known as lymphedema.
After the substance has been injected, the sentinel node(s) can be found either by using a special machine to detect radioactivity in the nodes, or by looking for nodes that have turned blue. To double check, both methods are often used. The surgeon then removes the node(s) containing the dye or radioactivity.
Sentinel lymph node mapping may be considered for certain cases of stage I cervical cancer. It is best used for tumors that are less than 2 cm in size. If your surgeon is planning sentinel lymph node biopsies, you should discuss if this procedure is appropriate for you.
Even if sentinel lymph node mapping does not show any lymph nodes to biopsy, the surgeon will most likely still remove the lymph nodes on that side of the pelvis to make sure cancer is not missed. Also, any enlarged or suspicious lymph nodes need to be removed at the time of surgery, even if they do not map with dye.
More information about Surgery
For more general information about surgery as a treatment for cancer, see Cancer Surgery.
To learn about some of the side effects listed here and how to manage them, see Managing Cancer-related Side Effects.
- Written by
- References

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as journalists, editors, and translators with extensive experience in medical writing.
Eifel P, Klopp AH, Berek JS, and Konstantinopoulos A. Chapter 74: Cancer of the Cervix, Vagina, and Vulva. In: DeVita VT, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles and Practice of Oncology. 11th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2019.
Hoffman MS and Mann WJ. Cervical intraepithelial neoplasia: Procedures for cervical conization. UpToDate website. https://www.uptodate.com/contents/cervical-intraepithelial-neoplasia-procedures-for-cervical-conization. Updated December 11, 2018. Accessed September 5, 2019.
Jhungran A, Russell AH, Seiden MV, Duska LR, Goodman A, Lee S, et al. Chapter 84: Cancers of the Cervix, Vulva, and Vagina. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa: Elsevier; 2020.
Lécuru F, Mathevet P, Querleu D, et al. Bilateral negative sentinel nodes accurately predict absence of lymph node metastasis in early cervical cancer: results of the SENTICOL study. J Clin Oncol. 2011;29:1686-1691.
National Cancer Institute. Physician Data Query (PDQ). Cervical Cancer Treatment – Health Professional Version. 2019. https://www.cancer.gov/types/cervical/hp/cervical-treatment-pdq. Updated February 6, 2019. Accessed on September 5, 2019.
National Comprehensive Cancer Network (NCCN). Clinical Practice Guidelines in Oncology: Cervical Cancer. Version 5.2019. Accessed at https://www.nccn.org/professionals/physician_gls/pdf/cervical.pdf on December 12, 2019.
Park DA, Yun JE, Kim SW, Lee SH. Surgical and clinical safety and effectiveness of robot-assisted laparoscopic hysterectomy compared to conventional laparoscopy and laparotomy for cervical cancer: A systematic review and meta-analysis. Eur J Surg Oncol. 2016;S0748-7983(16)30687-4.
Shepherd JH, Spencer C, Herod J, Ind TEJ. Radical vaginal trachelectomy as a fertility-sparing procedure in women with early-stage cervical cancer--cumulative pregnancy rate in a series of 123 women. BJOG. 2006; 113:719-723.
Taylor NP. Cervical intraepithelial neoplasia: Ablative therapies. UpToDate website. https://www.uptodate.com/contents/cervical-intraepithelial-neoplasia-ablative-therapies. Updated December 28, 2017. Accessed September 5, 2019.
Willows K, Lennox G, Covens A. Fertility-sparing management in cervical cancer: balancing oncologic outcomes with reproductive success. Gynecol Oncol Res Pract. 2016; Oct 21; 3:9. eCollection.
Last Revised: January 3, 2020
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.


